Call Us Today!
(808) 359-2276
Losing a tooth can affect more than appearance — it changes how you bite, speak, and feel about smiling. Implant restorations are designed to rebuild those essential functions while producing a natural-looking result. Unlike removable options that can shift during chewing or speaking, implant-supported restorations anchor to the jaw and behave much like natural teeth, helping patients regain everyday comfort and confidence.
This treatment option suits a wide range of situations, from replacing a single missing tooth to stabilizing a full denture. Because the restoration is attached to a titanium post integrated into the jawbone, it delivers stability and forces the bone to maintain its shape and strength. The preservation of jawbone is a major reason many patients choose implants over other restorative routes.
At the office of Kahana Family Dental Center we emphasize personalized planning; the ideal restoration balances function, aesthetics, and long-term oral health. Your dentist will assess your bite, jawbone health, and cosmetic goals to determine the most appropriate implant solution for your smile.
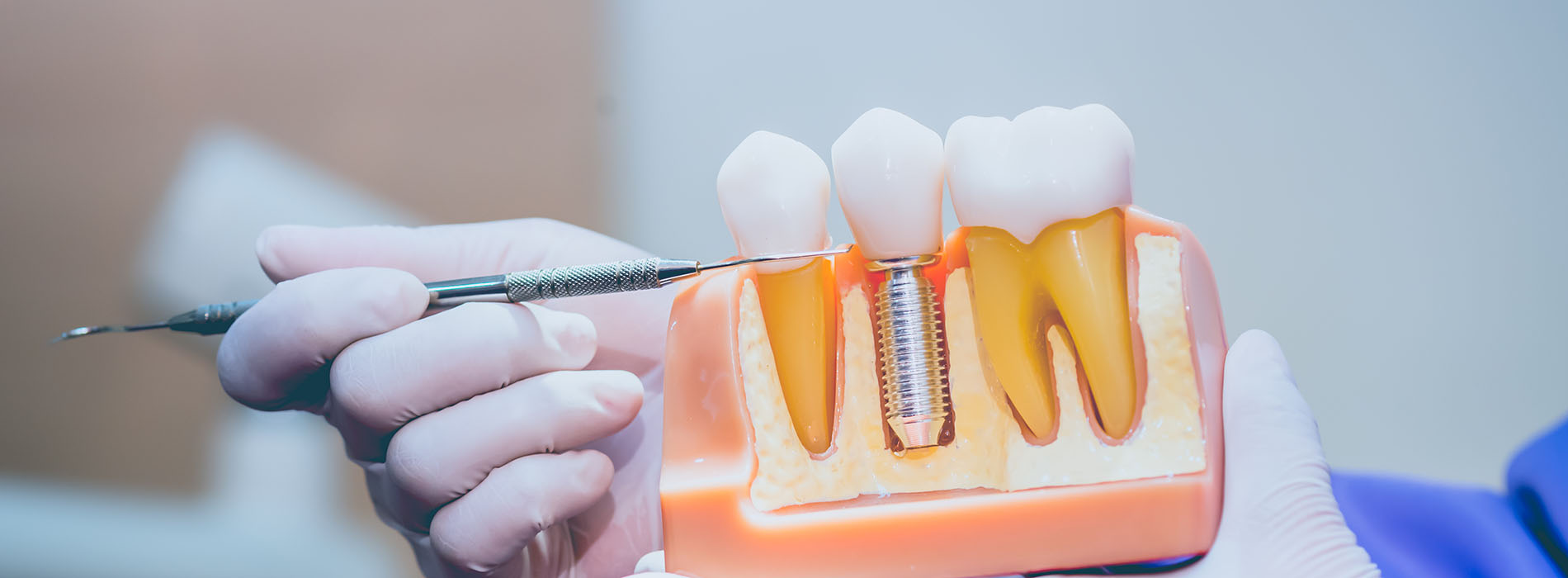
A dental implant begins as a small, biocompatible post placed within the jawbone where a tooth is missing. Over time, the bone grows around the post in a process called osseointegration, creating a secure foundation similar to a natural tooth root. Once integrated, the implant can support crowns, bridges, or attachments for removable prostheses.
Implants are typically made from titanium or other materials tested for compatibility with human tissues. Their design and material encourage bone cells to attach to the surface, which is why implants provide long-term stability rather than simply resting on the gums. This root-like function helps preserve facial structure and reduces the gradual bone loss that can occur after tooth extraction.
Importantly, implant restorations restore not only the look of a tooth but also the ability to bite and chew effectively. For many patients, this translates into improved nutrition, clearer speech, and a more confident social life — all outcomes that extend beyond oral health into overall well-being.
The path to a finished implant restoration usually involves several coordinated steps. First, your dentist evaluates the health of your gums and jawbone with a clinical exam and imaging to confirm that the site is suitable for implant placement. If additional preparatory work is needed — such as bone grafting or gum treatment — these procedures are planned to create a stable foundation.
Next, the implant post is placed during a minor surgical appointment. Local anesthesia and modern sedation options keep the experience comfortable for most patients. After placement, a healing period follows to allow the implant to integrate with the bone; the exact length varies by individual factors like bone quality and overall health.
When integration is complete, an abutment is attached and impressions are taken for the final restoration. Your dentist and dental lab craft a crown, bridge, or denture to match the color, shape, and function of your existing teeth. The final restoration is then secured to the implant, restoring chewing function and a natural appearance.
One clear advantage of implant-supported restorations is their longevity. When properly cared for, implants can last many years because they closely mimic the structure and load-bearing properties of natural teeth. This contrasts with some conventional bridges or removable dentures, which may need more frequent repair or adjustment over time.
Implants also protect surrounding teeth in ways that fixed bridges do not. Traditional bridges often require altering adjacent healthy teeth to serve as anchors, while implant restorations allow those teeth to remain untouched. This conservative approach helps preserve natural tooth structure and reduces the risk of future dental work on neighboring teeth.
From a functional standpoint, implants deliver superior chewing efficiency and stability. Patients typically notice easier eating and clearer speech, since implant restorations do not slip or require adhesives. For many people, these improvements make daily life more comfortable and help sustain better oral hygiene routines.
Proper care is essential to keep implant restorations performing well for the long term. Daily brushing and flossing around the implant area help prevent plaque buildup and gum inflammation, which are the leading threats to the tissues supporting an implant. Your dental team will demonstrate the most effective techniques and recommend tools — such as interdental brushes or water flossers — when appropriate.
Regular professional checkups are equally important. During routine visits, your dentist will examine the implant, surrounding gum tissue, and bite to catch early signs of wear or irritation. Periodic cleanings remove hardened deposits that at-home care can miss and ensure the restoration stays healthy and attractive.
Patients who maintain good oral hygiene and attend scheduled dental visits enjoy the best prognosis for long-term implant success. Lifestyle factors such as tobacco use and uncontrolled systemic conditions can affect outcomes, so open communication with your provider about your health and habits helps the team tailor preventive measures and follow-up care.
If questions arise at any stage — from daily maintenance to signs of sensitivity or change — your dental team is your best resource for guidance. Prompt evaluation of concerns helps protect both the implant and your overall oral health.
Summary — rebuilding your smile with confidence: Implant restorations offer a reliable, natural-feeling solution for replacing missing teeth while protecting the health and appearance of your jaw and remaining teeth. With thoughtful planning, careful placement, and ongoing care, implant-supported crowns, bridges, and dentures can restore function and improve quality of life. To learn more about whether implant restorations are the right choice for you, please contact us for additional information.
Implant restorations are prosthetic teeth that are secured to dental implants, small biocompatible posts placed in the jawbone to replace missing tooth roots. Over time the bone integrates with the implant in a process called osseointegration, creating a stable foundation similar to a natural tooth root. Once integrated, the implant can support crowns, bridges, or attachments for removable prostheses to restore chewing function and appearance.
The office of Kahana Family Dental Center emphasizes planning that balances function, aesthetics, and long-term oral health when designing an implant restoration. Restorations are customized to match adjacent teeth in color and shape so the final result looks natural and performs like a biological tooth. Because the restoration is anchored to bone, it provides greater stability than removable options and helps maintain jawbone structure.
Candidates for implant restorations typically include people with one or more missing teeth who have adequate jawbone volume and healthy gums. A comprehensive exam, including clinical evaluation and imaging, helps determine whether the bone and soft tissue can support an implant or whether preparatory procedures such as bone grafting or periodontal treatment are needed. Your dentist will also review medical history and any systemic conditions to assess how they may affect healing and implant success.
Even patients with controlled chronic conditions or past dental challenges can often proceed with implants after appropriate planning and coordination of care. Lifestyle factors such as tobacco use and certain medications can influence outcomes, so honest discussion with your provider helps the team tailor recommendations. If implants are not immediately feasible, alternative restorative approaches can be considered while preparing the mouth for future implant therapy.
The timeline for an implant restoration varies by case but generally follows a multi-step process that includes consultation, implant placement, healing, and final restoration. After the implant is placed, a healing period allows osseointegration to occur; this period commonly spans several weeks to a few months depending on bone quality and individual healing. Once the implant is stable, an abutment is attached and impressions are taken for the laboratory to fabricate the final crown, bridge, or denture.
Some situations allow for immediate provisional restorations or accelerated protocols, but these depend on clinical factors and should be discussed with your dentist. Close monitoring during the healing phase ensures the implant integrates properly and any necessary adjustments are made before finalizing the restoration. Your dental team will provide a personalized timeline and explain each stage so you know what to expect.
Implant posts are most often made from titanium or titanium alloys because of their proven biocompatibility and ability to integrate with bone. Abutments, which connect the implant to the visible restoration, can be metal or ceramic, and final crowns and bridges are commonly crafted from porcelain-fused-to-metal, all-ceramic materials like zirconia, or high-strength porcelains. Material selection is guided by factors such as strength requirements, aesthetic goals, and the location of the missing tooth.
Modern restorative materials are designed to mimic the translucency and color of natural teeth while providing durability for normal chewing forces. Dental laboratories work with the dentist to customize shape, shade, and surface texture so the restoration blends with the surrounding dentition. Your dentist will explain the advantages of specific materials and recommend the best option for your functional and cosmetic needs.
Implant restorations differ from traditional bridges and removable dentures in how they are supported and how they affect surrounding structures. Unlike bridges that rely on adjacent teeth for support, implants are anchored in bone and typically do not require altering neighboring healthy teeth, which helps preserve natural tooth structure. Compared with removable dentures, implant-supported restorations provide improved stability, chewing efficiency, and comfort because they do not slip or rely on adhesives.
Implants also help preserve jawbone by transmitting chewing forces into the bone, which reduces the bone loss that can occur after tooth extraction and with conventional dentures. While each restorative option has clinical indications, implants are often preferred when the goal is long-term function and bone preservation. Your dentist will evaluate your oral health needs and preferences to determine the most appropriate treatment plan.
As with any surgical procedure, implant placement carries potential risks that include infection, impaired healing, and in rare cases nerve injury or sinus complications when upper jaw implants extend into the sinus area. Peri-implantitis, an inflammatory condition affecting the tissues around an implant, can occur if plaque accumulates and is not managed effectively. Careful planning, sterile surgical technique, and good oral hygiene are essential to minimize these risks.
Most complications are preventable or manageable when detected early through routine follow-up visits and professional cleanings. Patients with certain systemic conditions or lifestyle factors may require additional medical coordination or modified protocols to reduce the chance of adverse outcomes. Open communication with your dental team about symptoms such as persistent pain, swelling, or mobility helps ensure prompt evaluation and appropriate care.
Maintaining implant restorations requires the same daily commitment as natural teeth, including thorough brushing twice a day and cleaning between teeth once a day with floss, interdental brushes, or a water flosser. Gentle techniques and nonabrasive toothpaste help protect restorative surfaces, and special interdental aids can be recommended for hard-to-reach areas around the implant. Consistent home care reduces plaque buildup and lowers the risk of inflammation around the implant.
In addition to home care, regular professional checkups and periodontal maintenance are vital to monitor tissue health and remove biofilm that cannot be eliminated at home. Your dental team will demonstrate the best cleaning methods for your specific restoration and schedule recall visits appropriate to your needs. Prompt attention to changes such as tenderness, redness, or looseness gives the clinician the best chance to intervene early and protect the implant.
Implant restorations are designed to closely replicate the appearance and function of natural teeth, with crowns and bridges customized to match the color, shape, and contours of adjacent teeth. Because the restoration is securely attached to the implant, chewing efficiency and stability often approach that of a natural tooth, allowing comfortable eating and clear speech. The sensation is different from natural teeth because implants lack a periodontal ligament, but most patients adapt quickly and report high satisfaction with function.
A restorative dentist and dental laboratory collaborate to achieve an aesthetic outcome that complements your smile and facial features. Minor adjustments to the bite or contours may be made after the restoration is placed to ensure comfort and proper function. If esthetic concerns arise, discuss refinements with your provider so the final result meets both functional and cosmetic expectations.
Yes. One of the key benefits of implant restorations is their ability to help preserve jawbone by transmitting normal chewing forces into the bone where the implant is placed. This mechanical stimulation encourages bone maintenance and reduces the bone resorption that commonly follows tooth loss, which in turn helps support facial contours and prevent the sunken appearance associated with long-term tooth loss. By acting like a tooth root, an implant helps maintain the height and density of the surrounding bone.
Timely replacement of missing teeth with implants or appropriate restorative solutions contributes to longer-term oral health and prosthetic stability. Preservation of bone also provides a more stable foundation for future restorative care if additional treatment becomes necessary. Discussing timing and planning with your dentist ensures that bone preservation is considered when developing a comprehensive treatment plan.
Before surgery you can expect a thorough evaluation and treatment plan that includes imaging and discussion of anesthesia or sedation options to ensure comfort during the procedure. Implant placement is a minor surgical procedure typically performed under local anesthesia and, when appropriate, conscious sedation; most patients experience manageable discomfort afterward that is controlled with prescribed medications and standard post-operative care such as ice and rest. Your dentist will provide specific aftercare instructions and schedule follow-up visits to monitor the healing process.
During the healing phase it is important to follow dietary and hygiene recommendations to support osseointegration, and temporary restorations may be used to maintain appearance and function while the implant integrates. Once integration is confirmed, the final abutment and restoration are placed and minor adjustments are made to ensure proper fit and bite. If you have questions or concerns at any point, contact Kahana Family Dental Center so the team can provide guidance and timely evaluation.
