Call Us Today!
(808) 359-2276
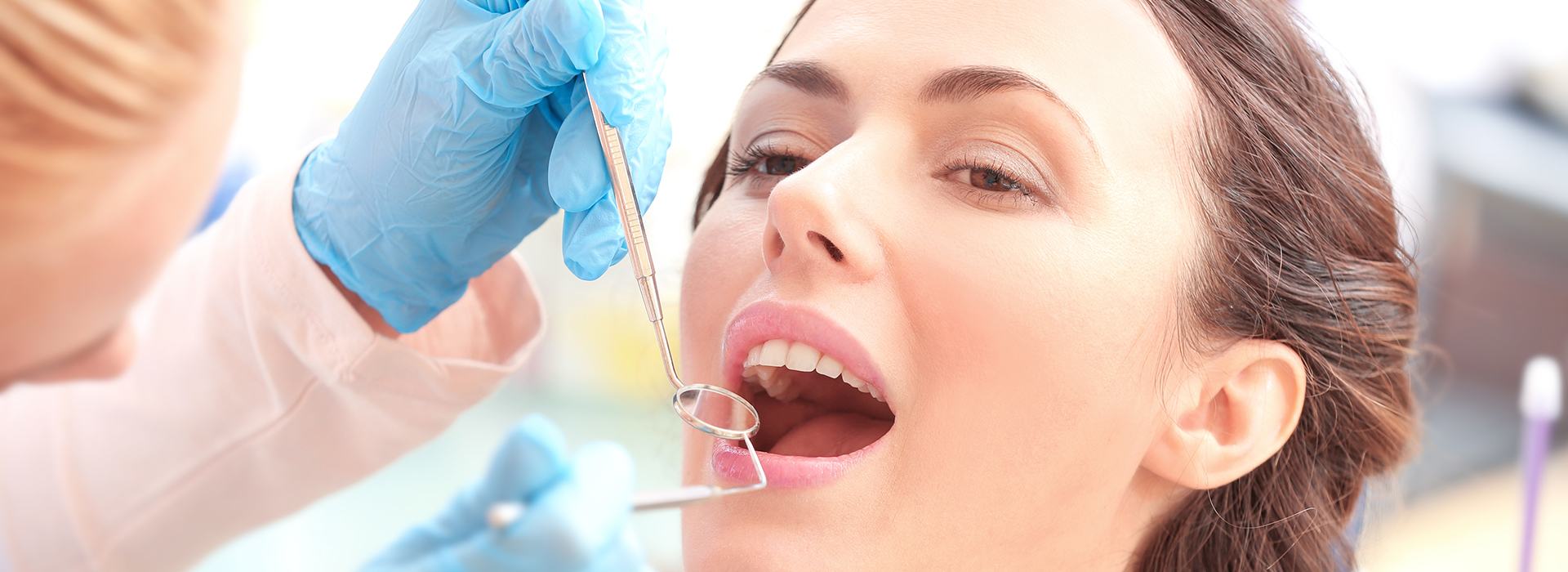
Gum disease is the leading cause of tooth loss in adults — and it often advances quietly. Studies from major public health organizations indicate that roughly half of Americans aged 30 and older show signs of periodontal disease. Fortunately, most cases are preventable or manageable when detected early. At the office of Kahana Family Dental Center, we provide a full spectrum of periodontal care designed to protect the tissues that hold your teeth in place and to help you keep a healthy, confident smile for years to come.
Healthy gums do more than frame an attractive smile — they are essential to your overall oral function and comfort. Inflammation and infection of the supportive tissues (the periodontium) gradually erode the connections that stabilize teeth. Over time, this can lead to shifting, loose teeth, and ultimately tooth loss if left unchecked.
Researchers increasingly recognize links between chronic oral inflammation and systemic health concerns, such as cardiovascular disease and poorly controlled diabetes. While the exact relationships are complex, minimizing oral inflammation through effective periodontal care is a meaningful step toward better whole-body health.
Prevention and early intervention are the cornerstones of periodontal wellness. Regular professional assessments combined with effective home care allow our team to identify changes early and recommend treatments tailored to the specific stage and activity of disease in each patient.
Periodontal disease does not always cause pain, which is why paying attention to subtle signs can make a critical difference. Noticing bleeding during brushing or flossing, persistent bad breath, or a change in how your teeth fit together are common early indicators that a closer look is needed.
Because symptoms vary from person to person, routine dental exams are the best way to catch the disease before it progresses. During a periodontal evaluation, measurements of pocket depth, assessment of gum recession, and checks for bone loss allow clinicians to form a precise picture of your oral health.
Below are common symptoms that can signal a periodontal problem. If you experience any of these, scheduling an evaluation can help protect your long-term dental health:
Red, swollen, or tender gums
Bleeding while brushing, flossing, or eating
Gums pulling away from teeth or exposed root surfaces
Increased sensitivity to hot, cold, or sweets
Persistent unpleasant mouth odor or taste
Sensation of teeth becoming loose or shifting
New spaces forming between teeth or changes in your bite
Discomfort when biting or chewing food
Discharge or pus around the gumline
Partial dentures that no longer fit comfortably

The earliest, reversible stage of periodontal disease is gingivitis. At this point the inflammation is limited to the soft tissue and has not yet caused irreversible attachment or bone loss. Common signs include gum redness, swelling, and bleeding during routine oral care.
With timely attention — professional cleaning, improved oral hygiene, and routine monitoring — gingivitis can usually be controlled and reversed. This makes regular cleanings and honest home care practices the first line of defense for most people.
If gingivitis is not treated, the condition can progress to periodontitis. In periodontitis, the inflammatory process extends deeper, destroying connective tissue and bone that support the teeth. As pocketing deepens, bacteria become harder to remove and the risk of permanent damage increases.

Today’s periodontal treatment aims to arrest disease activity, reduce bacterial load, and restore an environment where tissues can remain healthy. The choice of therapy depends on disease severity, pocket depth, bone loss, and the patient’s overall health and preferences.
Non-surgical measures are frequently the first step. Thorough scaling and root planing removes plaque and hardened deposits below the gumline and smooths root surfaces to discourage reattachment of bacteria. These mechanical procedures, often combined with targeted antimicrobial strategies, can significantly reduce inflammation and pocket depth.
When deeper disease is present, surgical approaches may be necessary to gain access to root surfaces, recontour bone, or regenerate lost tissue. Modern periodontal surgery includes flap procedures, guided tissue regeneration, and grafting techniques that support both function and form. Minimally invasive options, including selected use of dental lasers, can also play a role in reducing pocket depth and managing difficult-to-reach areas.
When disease is identified early or is localized, conservative treatments are often effective. Scaling and root planing — sometimes supplemented with localized antimicrobial agents — reduce bacterial reservoirs and allow inflamed tissue to calm.
These procedures are performed with careful technique and attention to patient comfort. They are typically followed by a tailored home-care program and a maintenance schedule to monitor healing and prevent recurrence.
If non-surgical therapy does not produce sufficient improvement, the clinical team will discuss additional options aimed at stabilizing the condition and protecting tooth support.
For cases with deeper pockets, progressive bone loss, or anatomy that limits non-surgical access, periodontal surgery can provide definitive cleaning and repair. Flap procedures expose root surfaces for thorough debridement and allow reshaping of bone to reduce pocket depths.
Where tissue and bone have been lost, regenerative techniques such as bone grafts, soft-tissue grafts, and guided tissue regeneration can help rebuild support, improve stability, and enhance esthetics. These procedures are planned carefully to match clinical goals and patient expectations.
Advances in technology — including microsurgical tools and selective laser therapy — have expanded options for treating complex cases while focusing on predictable healing and patient comfort.
Eliminate bacteria and remove deposits below the gumline
Stabilize or rebuild underlying bone and soft tissues when feasible
Reduce pocket depth to make daily home care more effective and sustainable
Periodontal care does not end when initial therapy is complete. A customized maintenance program is essential to preserving gains and preventing recurrence. Maintenance intervals are set based on disease severity and individual risk factors; some patients benefit from visits every three months, while others remain stable with standard six-month recalls.
Effective maintenance combines professional monitoring and cleanings with realistic, patient-centered home-care strategies. We work with each person to develop a routine that fits their lifestyle and reduces risk factors such as smoking or poorly controlled medical conditions that can influence healing.
In many cases, periodontal treatment also supports other restorative goals. Regenerating bone and tissue can improve the prognosis for dental implants or other replacements, and thoughtful coordination between periodontal and restorative care helps optimize long-term outcomes.
Our approach is collaborative: we provide clear explanations of findings, treatment options, and expected results so you can make informed decisions about your care. Education, gentle treatment, and consistent follow-up create the best chances for long-term periodontal stability.
At the office of Kahana Family Dental, we combine modern techniques with a commitment to patient comfort and individualized care. Whether you are managing early gingivitis or a more advanced periodontal condition, we strive to protect your natural teeth and support overall oral health.
If you have questions about periodontal treatment or would like to learn more about protecting your gums and supporting tissues, please contact us for more information.
Most people don’t realize that periodontal disease is the leading cause of tooth loss among adults. According to statistics from the Centers for Disease Control and Prevention, one out of every two adults over the age of 30 in the United States has periodontal disease.
You may be surprised to learn that the human mouth is home to a wide variety of microbes. The fact is that over 700 different strains of bacteria have been detected in the oral cavity. Although some of these bacteria are beneficial, others are harmful to oral health. Without proper oral hygiene and routine dental care, these harmful bacteria can cause tooth decay and gum disease, compromising both your oral health and overall wellbeing.
In addition to inadequate oral hygiene and infrequent professional care, other factors, including smoking, genetic tendencies, and unchecked diabetes, can contribute to the escalation of periodontal disease.
Your gums and teeth have an interdependent relationship, which means healthy teeth depend on the support of healthy gums. Also, taking care of your smile does more than keep your teeth and gums in optimal condition; good oral health also supports systemic health. In addition to being the leading cause of tooth loss in adults, researchers are finding more and more links between periodontal disease and a number of medical problems, including heart disease, stroke, diabetes, respiratory problems, and adverse pregnancy outcomes such as pre-term and low birth-weight babies.
If you notice that your gums are bleeding with the slightest pressure while brushing or flossing, it’s a sign of gingivitis. Although gingivitis is the earliest stage of gum disease, it can easily be reversed with deeper cleanings as well as an improved regimen of oral hygiene at home.
In the absence of professional treatment and better home care, gingivitis progresses to the next stage, which is known as periodontitis. In this stage, the connective tissue and bone that hold the teeth in place begin to break down with an increase in pocketing between the teeth and bone, gum recession, and bone loss. Without proper treatment by your dentist, periodontitis will progress from a mild to moderate loss of supporting tissue to the destruction of the bone around the teeth.
Although gingivitis can often be reversed with improved oral hygiene and professional cleanings, as periodontal disease advances, more extensive procedures are required to halt its progression. Based on a complete assessment of your periodontal health and a review of possible contributing factors, our office will recommend the best options in care. Treatment for periodontitis may include a series of deeper cleanings known as root planing and scaling, surgical procedures to reduce pocket depth, bone or tissue grafts, laser procedures, or antimicrobial medications.
The cost of care depends on the type of procedures required to restore your periodontal health. If you have dental insurance, plans often cover treatment to prevent gum disease as well as many procedures to treat the various stages of gum disease. Our goal is to help patients restore and maintain good oral health. We do all we can to help you begin care without additional stress or delay. Our business office works with you to maximize your benefits and provide easier, more convenient payment options.
By seeing our office regularly for care and doing your best to eat a healthy diet and practice good oral hygiene, you can keep your smile in tip-top shape as well as protect your overall wellbeing.
At the office of Kahana Family Dental, we provide a comprehensive range of services to address all your oral healthcare needs. You can rest assured that your smile is in the best of hands at our office. Our skilled and experienced team maintains a position at the forefront of advances in care and remains dedicated to providing the highest quality of skilled and compassionate treatment.
Periodontal disease is an infection of the tissues that support the teeth caused by bacterial plaque that accumulates along the gumline. It begins as gingivitis, a reversible inflammation of the gum tissue, and can progress to periodontitis when the infection destroys connective tissue and bone. Without treatment, this progression undermines tooth stability and can ultimately lead to tooth loss.
Periodontal disease is common, and public health studies indicate roughly half of Americans aged 30 and older show signs of periodontal issues. Early stages often cause little or no pain, so routine dental exams are important for detection. When recognized early, most cases are preventable or manageable with appropriate care and monitoring.
The primary cause of gum disease is the buildup of bacterial plaque and hardened calculus on tooth surfaces near the gums, which triggers inflammation. Individual risk factors such as poor oral hygiene, tobacco use, uncontrolled diabetes, certain medications, and genetic predisposition can increase susceptibility. Changes in hormone levels and conditions that weaken immune response also contribute to disease progression.
Because risk varies by person, a comprehensive assessment helps identify specific contributing factors and guide treatment. Addressing modifiable risks—improving home care, quitting smoking, and managing medical conditions—greatly improves treatment outcomes. Regular professional care reduces the chance that early inflammation will become destructive disease.
Common warning signs include gums that bleed during brushing or flossing, persistent bad breath or an unpleasant taste, red or swollen gums, and gum recession that exposes root surfaces. Patients may also notice teeth that feel loose, new spaces between teeth, changes in bite, or discomfort when chewing. In some cases infection causes pus or discharge around the gumline.
Because periodontal disease can be painless in its early stages, any of these symptoms should lead to a professional evaluation rather than self-diagnosis. A timely assessment allows clinicians to measure pocket depths, check for gum attachment loss and bone changes, and design a treatment plan that matches disease severity. Early detection improves the likelihood of conservative, effective care.
Diagnosis begins with a thorough periodontal examination that includes probing pocket depths around each tooth, assessing gum recession and attachment loss, checking for bleeding on probing, and evaluating tooth mobility. Dental radiographs are used to detect bone loss and to document the extent and pattern of periodontal damage. The clinical picture, combined with medical and dental history, helps determine disease activity and risk.
Following diagnosis, clinicians create an individualized treatment plan that addresses the type and severity of disease as well as patient-specific risk factors. Periodontal charts and radiographs are used to monitor response to therapy over time and to adjust maintenance intervals. Clear communication of findings helps patients participate in decisions about their care.
Scaling and root planing (SRP) is a non-surgical, deep-cleaning procedure that removes plaque and hardened calculus from below the gumline and smooths root surfaces to discourage bacterial reattachment. SRP is frequently the first-line therapy for patients with early to moderate periodontitis or localized pockets that are difficult to clean with routine hygiene. The procedure promotes reduction of inflammation and allows the gum tissue to reattach more closely to the tooth surface.
In many cases SRP is combined with targeted antimicrobial strategies, such as localized delivery agents or short-term systemic therapy when clinically indicated. Healing is typically reassessed several weeks after treatment to determine whether pockets have improved or if additional intervention is needed. A tailored home-care routine and appropriate maintenance visits support long-term success after SRP.
Periodontal surgery is considered when non-surgical therapy fails to reduce pocket depths sufficiently, when there is progressive bone loss, or when anatomy limits access for thorough cleaning. Surgical procedures allow clinicians to gain direct access to root surfaces for debridement, reshape bone to reduce pocketing, and place regenerative materials where appropriate. The goal is to stop disease progression, reduce pocket depth, and restore a healthier environment for the tissues.
Specific surgical options include flap surgery for access and debridement, bone grafting and guided tissue regeneration to encourage regeneration of lost support, and soft-tissue grafts to correct recession. Advances in microsurgical techniques and selective laser therapy can enhance precision and patient comfort, but the choice of procedure depends on clinical findings and patient goals. Postoperative care and a committed maintenance program are essential for long-term stability.
Regenerative procedures aim to rebuild lost bone and connective tissue that support teeth by using bone grafts, barrier membranes, growth factors, or combinations of these approaches. These techniques are indicated when periodontal destruction has created defects that are likely to respond to regenerative therapy, such as localized vertical bone defects or areas where tissue support is insufficient. The objective is to improve tooth stability and create a better foundation for restorative work when needed.
Not every patient or defect is a candidate for regeneration; careful clinical and radiographic assessment determines the likelihood of predictable improvement. Regenerative therapy is often coordinated with restorative planning, particularly when future dental implants or long-term prosthetic solutions are being considered. Patients should understand the expected healing timeline and the importance of following postoperative and maintenance recommendations to protect the regenerated tissues.
Laser therapy and other minimally invasive techniques can be useful adjuncts in periodontal treatment, helping to reduce bacterial load, remove diseased tissue, or improve access in select clinical situations. These technologies may enhance patient comfort and reduce bleeding, but they are not a universal replacement for proven mechanical cleaning methods such as scaling and root planing. Their effectiveness depends on the type of laser, the specific indication, and the clinician's experience.
When used appropriately, minimally invasive approaches can complement traditional therapy and support wound healing, particularly in localized or shallow defects. The decision to use lasers or other advanced tools is made on a case-by-case basis after a careful evaluation of disease severity and treatment goals. Patients should discuss the expected benefits and limitations of these options with their dental provider.
After periodontal therapy, diligent home care is essential to protect healing tissues and prevent recurrence; this includes gentle but thorough brushing with a soft-bristled brush, daily interdental cleaning with floss or interdental brushes, and following any temporary recommendations such as antimicrobial rinses. Addressing risk factors such as tobacco use and uncontrolled medical conditions like diabetes improves healing and long-term outcomes. Your clinician will provide specific postoperative instructions tailored to the procedures you received.
Long-term success also depends on a structured maintenance program that typically includes professional periodontal cleanings and reassessments at intervals determined by disease severity and individual risk. At Kahana Family Dental Center we work with patients to create realistic home-care routines and maintenance schedules that fit their needs. Consistent follow-up and communication with the dental team help preserve gains achieved through treatment.
Periodontal health is foundational to many restorative and prosthetic dental procedures; controlling infection and stabilizing supporting tissues improves the prognosis for crowns, bridges, dentures, and dental implants. Treating periodontal disease before placing definitive restorations reduces the risk of future complications and supports predictable long-term results. Coordination between periodontists, general dentists, and restorative specialists ensures treatment sequencing that aligns with each patient's goals.
Periodontal inflammation can also have implications for overall health, and care providers may coordinate with a patient's physician when systemic conditions such as diabetes or cardiovascular disease are present. At Kahana Family Dental Center we emphasize collaborative, evidence-based care and clear communication so oral treatment plans support broader health objectives. Maintaining periodontal stability through treatment and regular maintenance contributes to both oral and general well-being.
